This Common Habit Can Cause Oral Cancer (Most People Ignore It)
By Dr. Supreet Bhatt | Head & Neck Cancer Surgeon, Ahmedabad | Last Updated: March 2026
Most people who chew gutka or paan every day do not think of it as a health risk. It is too common. Too normal. Roadside shops sell it openly. Colleagues do it after lunch. It has been part of daily life for decades.
That normalcy is exactly why oral cancer catches so many people off guard.
India records more cases of oral cancer linked to smokeless tobacco and areca nut than any other country in the world. Yet the majority of patients who walk into a surgeon's clinic arrive late - at Stage III or Stage IV - because they dismissed the early signs for months, sometimes years.
This article covers what oral cancer is, why that one common habit is responsible for so many cases in India, the early warning signs you should never ignore, and when it is time to see a specialist.
What Is Oral Cancer?
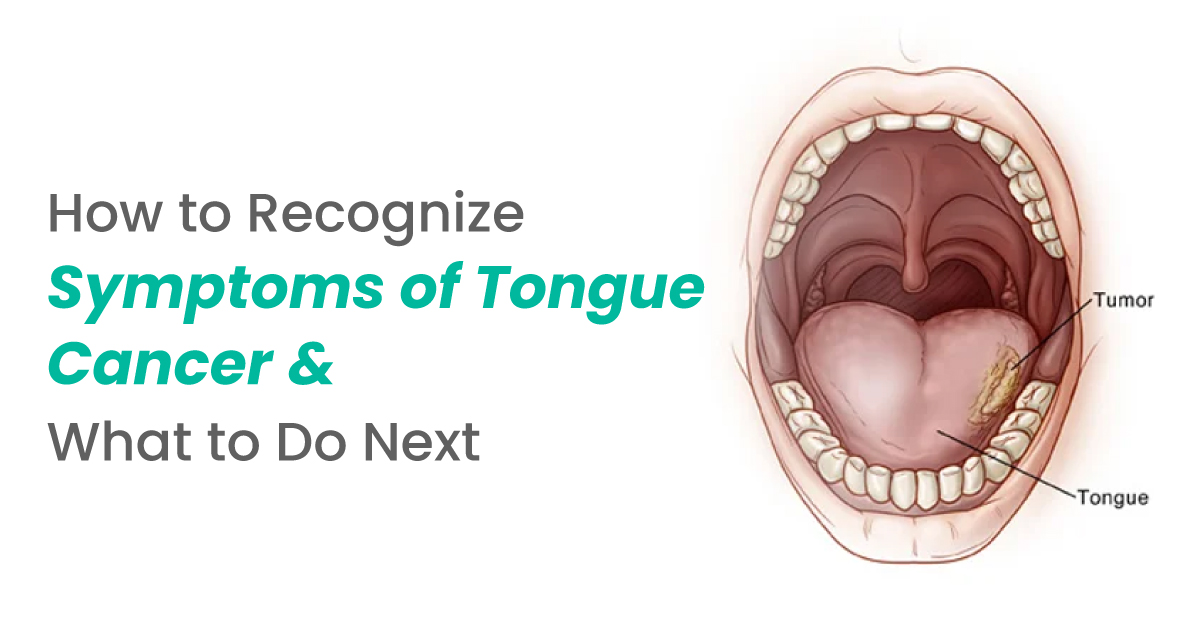
Oral cancer is cancer that starts in the tissues of the mouth. It can develop on the lips, tongue, the floor of the mouth, the gums, the inner lining of the cheeks, the hard palate (roof of the mouth), or the area just behind the wisdom teeth.
Most oral cancers are a type called squamous cell carcinoma. Squamous cells are the flat, thin cells that line the inside of your mouth. When these cells accumulate DNA damage over time - from tobacco, chemicals, chronic irritation - some of them begin to grow uncontrollably. That uncontrolled growth is cancer.
Oral cancer is the most common form of head and neck cancer in India. It is roughly twice as common in men as in women, and most cases are diagnosed in people over 40. But cases in younger people are rising, partly because habits like gutka chewing often start in adolescence.
Where does oral cancer most commonly develop?
The tongue (especially the sides and undersurface) and the floor of the mouth are the two most frequent sites. The inner cheeks are also common - particularly in people who chew gutka and hold it in one spot for long periods.
It is worth distinguishing oral cavity cancer from oropharyngeal cancer. Oropharyngeal cancer develops at the back of the throat - the tonsils, the base of the tongue, the soft palate. It is often linked to HPV (human papillomavirus) rather than tobacco. Both fall under the broader category of head and neck cancer, but they behave differently and require different treatment approaches.
The Common Habit That Causes Oral Cancer
Here is the uncomfortable truth: for most Indians who develop oral cancer, the cause is not cigarettes. It is not alcohol. It is a habit so common that many people do not even register it as tobacco use.
It is chewing gutka, khaini, paan with tobacco, mawa, or plain areca nut (supari) - often starting as a mild habit and, over years, becoming something done ten, fifteen, twenty times a day.
Why gutka and paan chewing cause oral cancer
Smokeless tobacco is not safer than smoked tobacco. It contains over 28 known carcinogens, including tobacco-specific nitrosamines (TSNAs), formaldehyde, and cadmium. When you hold gutka or khaini in your mouth, these chemicals are in direct, prolonged contact with the mucosal lining. Over months and years, they cause repeated DNA damage in the squamous cells lining your mouth.
Areca nut - the nut inside every paan and paan masala product - is classified as a Group 1 carcinogen by the International Agency for Research on Cancer (IARC). That is the same category as tobacco smoke, asbestos, and formaldehyde. This applies to areca nut even when there is no tobacco in the product.
One of the most serious consequences of long-term gutka chewing is oral submucous fibrosis (OSMF) - a pre-cancerous condition where the inside of the mouth gradually becomes stiff and fibrous. People with OSMF often notice they cannot open their mouth as wide as they used to. The tissue feels tight and burns when eating spicy food. OSMF itself does not mean cancer has developed, but it is a direct warning that the tissue has been severely damaged. Without stopping the habit and getting proper treatment, OSMF progresses to oral cancer in a significant proportion of cases.
The numbers from India
A 2024 data analysis of oral cavity cancer patients in India found that gutka use was the most prevalent tobacco habit, present in over 54% of cases - and patients with gutka use were more likely to be diagnosed with advanced-stage tumours (T4 lesions) than non-gutka users.
Broader national data from the Indian Council of Medical Research (ICMR) and IARC consistently shows:
- Among Indian men: khaini accounts for the highest proportion of oral cancer cases, followed by gutka and betel quid with tobacco
- Among Indian women: areca nut and betel quid with tobacco are the primary drivers
- The habit typically begins in the mid-teens and the cancer diagnosis arrives 15 to 25 years later - which is why the "it hasn't harmed me yet" reasoning is so dangerous
Why people don't stop
Two things make this habit especially difficult to break. First, areca nut is genuinely addictive - it contains arecoline, a stimulant that produces a mild, short-lived euphoric effect. Second, products like paan masala are marketed aggressively as "mouth fresheners," which frames a known carcinogen as a hygiene product. Many users, particularly in smaller towns and semi-urban areas, simply do not know that plain paan masala without tobacco is still carcinogenic.
There is no safe level of gutka or areca nut consumption. Even one packet a day, over years, carries real risk. The dose makes the poison — but the poison is always present.
Other Risk Factors for Oral Cancer
Smokeless tobacco is by far the dominant risk factor for oral cancer in India, but it is not the only one. A complete picture includes:
Smoking: Cigarettes, bidis, and cigars all contain carcinogens that affect oral tissue directly. Heavy smokers have roughly six times the oral cancer risk of non-smokers. The risk multiplies sharply when smoking is combined with alcohol.
Alcohol: Regular heavy drinking damages the protective lining of the mouth and makes it more permeable to carcinogens. People who drink heavily and smoke heavily face oral cancer rates 30 times higher than non-users of either.
HPV (Human Papillomavirus): HPV type 16 is now associated with about 70% of oropharyngeal cancers in Western countries, and the proportion is rising in India too. HPV-linked oral cancer tends to affect younger, non-smoking patients - which is partly why we are seeing more oral cancer cases in people in their 30s.
Chronic oral irritation: A tooth with a sharp broken edge, an ill-fitting denture, or a poorly made dental cap that constantly rubs against the cheek can cause repeated tissue injury over years. On its own this is a relatively minor risk factor, but combined with tobacco use it matters.
Prolonged sun exposure: Mainly relevant to cancer of the lower lip, which is more common in people who work outdoors.
Poor nutrition: Diets lacking in fruits and vegetables are associated with higher oral cancer risk, likely because of reduced antioxidant intake.
Family history: A first-degree relative with oral or another head and neck cancer slightly increases risk, suggesting some inherited susceptibility.
None of these factors, individually, carries the same population-level impact as gutka and smokeless tobacco in India. But they combine. A person who chews gutka, smokes bidis, and drinks regularly is not facing three separate risks - those risks multiply each other.
Early Warning Signs of Oral Cancer You Should Never Ignore
This is the section that matters most, practically speaking. Oral cancer caught at Stage I or Stage II has treatment outcomes that are far better than cancer caught at Stage IV. The difference between those outcomes often comes down to how quickly someone acts on a symptom.
The problem is that early oral cancer rarely hurts. Pain is usually a late sign. People feel a sore or a patch and assume it will go away. Sometimes they are right - most mouth sores are harmless and heal in a week or two. The question is what happens when they do not.
The 2-week rule
Any symptom in the mouth that does not resolve within two weeks needs to be evaluated by a doctor or specialist. Not next month. Not after one more round of "wait and see." Two weeks.
Specific symptoms to watch for
A sore or ulcer that won't heal. The most common early sign. Most mouth ulcers from biting your cheek or eating something sharp heal in 7 to 10 days. A sore that stays beyond two weeks - especially if it is painless - should be examined.
White patches inside the mouth (leukoplakia). Flat or slightly raised white patches that cannot be wiped off. Some are benign, some are pre-cancerous, some are early cancer. You cannot tell by looking. A biopsy is needed.
Red patches (erythroplakia). Less common than white patches but actually higher risk. A bright red, velvety patch inside the mouth that cannot be explained by irritation or infection needs prompt evaluation.
Restricted mouth opening. If you notice over time that you cannot open your mouth as wide as before - cannot comfortably bite into an apple, or your jaw feels tight - this is a cardinal sign of oral submucous fibrosis (OSMF) from areca nut or gutka chewing. It is a pre-cancerous condition that needs treatment now.
A lump or thickening in the mouth or neck. A lump anywhere inside the mouth or a persistent swelling in the neck (which may indicate lymph node involvement) is a reason to see a specialist promptly.
Unexplained bleeding from the mouth. Not from brushing too hard. Bleeding from tissue in the mouth that has no obvious cause.
Numbness or persistent pain in the mouth, face, or neck with no clear dental or other explanation.
Difficulty chewing or swallowing. Or the sensation that food is getting stuck.
Persistent hoarseness or sore throat that is not explained by a cold or other infection and does not improve after a couple of weeks.
Loose teeth with no apparent dental cause — especially if accompanied by swelling of the surrounding gum.
A word about "waiting to see if it gets worse"
Many patients who come in late say the same thing: "I thought it would go away on its own." Some add: "It didn't hurt, so I didn't think it was serious." Both of these responses are understandable. Both of them cost time that matters in cancer treatment.
Early oral cancer is quiet. It does not announce itself with severe pain. That silence is not reassurance - it is just the early stage of the disease.
How Oral Cancer Progresses - Stages at a Glance
Doctors stage oral cancer on a scale of I to IV based on tumour size and whether it has spread.
| Stage | What it means | Treatment approach |
|---|---|---|
| Stage I | Tumour ≤ 2 cm, no lymph node involvement | Surgery alone, often successful |
| Stage II | Tumour 2–4 cm, no lymph node involvement | Surgery, possible radiation |
| Stage III | Tumour > 4 cm, or one nearby lymph node affected | Surgery + radiation or combined therapy |
| Stage IV | Tumour invades adjacent structures, multiple lymph nodes, or distant spread | Multimodal treatment; outcomes more challenging |
The data from Indian cancer registries consistently shows that 60% or more of oral cancer patients in India are diagnosed at Stage III or IV. This is not because the cancer is aggressive and fast-moving in early stages - it is because the early symptoms are ignored or misidentified.
The clinical reality is that a Stage I oral cancer treated surgically by an experienced head and neck surgeon has a very different outcome than the same cancer caught at Stage IV. Early detection is genuinely the intervention that changes survival.
How Is Oral Cancer Diagnosed?
Diagnosis starts with a physical examination. A head and neck surgeon or oral physician will examine your entire mouth systematically - lips, tongue (including the underside), floor of the mouth, cheeks, palate, gums - and palpate the lymph nodes in your neck.
If there is a suspicious lesion, a biopsy is performed. A small piece of tissue is removed from the area and examined under a microscope by a pathologist. This is the only definitive way to diagnose oral cancer. Biopsies of oral lesions are usually done under local anaesthesia and take only a few minutes.
If cancer is confirmed, imaging studies - CT scan, MRI, and in some cases a PET scan - are used to determine the size of the tumour, whether it has grown into surrounding structures, and whether lymph nodes or distant organs are involved. This staging determines the treatment plan.
One thing worth knowing: oral cancer screening during a routine dental check-up takes under five minutes and involves no needles, no radiation, and no recovery time. If you have been using gutka, paan, or tobacco for years, asking your dentist to do a quick oral screening at every visit is a reasonable step.
Oral Cancer Treatment Options
Treatment depends on the stage of cancer, the location of the tumour, and the patient's overall health. For most cases, surgery is the primary treatment.
Surgery involves removing the tumour and a margin of healthy tissue around it. If the cancer has reached nearby lymph nodes, a procedure called a neck dissection is performed to remove the affected nodes. In early-stage oral cancer, surgery alone is often sufficient.
Radiation therapy uses targeted high-energy beams to kill cancer cells. It is used after surgery when there is a risk of residual disease, or as the primary treatment when surgery is not suitable.
Chemotherapy is usually combined with radiation (called chemoradiation) rather than used alone. It makes cancer cells more sensitive to radiation and is used for locally advanced disease.
Targeted therapy and immunotherapy are newer options used for recurrent or metastatic oral cancer that does not respond to standard treatment.
Reconstruction is an important part of surgery for oral cancer. When a significant portion of the tongue, jaw, or floor of the mouth is removed, reconstructive surgery - often using tissue transferred from the arm, thigh, or chest - is performed at the same time to restore function and appearance.
For anyone dealing with a diagnosis or worried about symptoms, speaking with a specialist who focuses specifically on head and neck cancers makes a significant difference in the quality of evaluation and the range of options discussed.
How to Reduce Your Risk of Oral Cancer
Stop the habit - fully. Not cutting down. Stopping. This applies to gutka, khaini, paan with tobacco, mawa, paan masala, and plain areca nut. There is no safe version. The risk begins to decline after cessation, but the process is slow. The sooner you stop, the better the outcome.
Quit smoking and limit alcohol. If you use both, the combined effect is not additive - it is multiplicative. Stopping tobacco is the single most impactful thing you can do for oral cancer risk.
Get vaccinated against HPV. The HPV vaccine is now available in India and is recommended for both boys and girls, ideally before they become sexually active. It reduces the risk of HPV-related oropharyngeal cancer substantially.
See a dentist every 6 months. A significant number of oral cancers are found during routine dental examinations before the patient has noticed any symptoms. Regular dental visits are, in effect, oral cancer screenings.
Self-examine your mouth monthly. With a good light and a mirror, check the inside of your cheeks, the underside of your tongue, the floor of your mouth, and your gums. You are looking for white patches, red patches, lumps, sores, or anything that looks different from last month.
Eat more fruits and vegetables. The evidence on diet and oral cancer is not definitive, but diets rich in antioxidants - from food, not supplements - are consistently associated with lower cancer risk across multiple studies.
Use SPF lip protection outdoors if you work or spend significant time in the sun.
Frequently Asked Questions About Oral Cancer
Is gutka the main cause of oral cancer in India?
In the Indian context, yes - smokeless tobacco products including gutka, khaini, and betel quid with tobacco account for the largest share of oral cancer cases. National and international data consistently identify these habits as the primary drivers. Gutka alone was the most common habit reported in patients diagnosed with oral cavity cancer in recent Indian studies.
What are the first signs of oral cancer?
The most common early sign is a mouth sore or ulcer that does not heal within two weeks. White patches (leukoplakia) or red patches inside the mouth are also early warning signs, as is difficulty opening the mouth fully in people who use gutka or paan. None of these symptoms are necessarily painful in the early stages - waiting for pain before seeking evaluation is a mistake.
Can oral cancer be cured if caught early?
Yes. Stage I and Stage II oral cancer treated surgically have significantly better outcomes than advanced-stage cancer. Early detection genuinely changes what is possible in terms of treatment and recovery. This is why acting on symptoms within two weeks - rather than waiting to see if they resolve - matters.
Is paan masala without tobacco safe?
No. Areca nut - the main ingredient in paan masala - is classified as a Group 1 carcinogen by IARC regardless of whether tobacco is present. Products sold as "tobacco-free paan masala" still contain areca nut and still carry cancer risk. The "no tobacco" label is not the same as "safe."
When should I see a doctor for mouth symptoms?
If a sore, patch, swelling, or any unusual change in your mouth does not resolve within two weeks, see a doctor or dental professional. Do not wait for the symptom to become painful. Many early oral cancers are found precisely because someone acted on a painless symptom before it progressed.
Who is a head and neck cancer specialist?
A head and neck surgical oncologist is a surgeon who specialises in diagnosing and treating cancers of the mouth, throat, salivary glands, thyroid, and related structures. If you have symptoms that concern you, or if you have been using tobacco products for years and want a thorough evaluation, a head and neck specialist is the right person to see - not a general physician or dentist alone, though they can refer you.
The Bottom Line
Oral cancer is one of the most preventable cancers we know of. In India, the majority of cases are directly linked to a habit - chewing gutka, khaini, paan - that people start young and continue for decades without giving it a second thought.
The warning signs are real. They appear earlier than most people realise. And they are often quiet - no dramatic pain, no obvious alarm - which is precisely why so many people ignore them until the disease has advanced.
If you have been chewing gutka or paan for years, or if you or someone you know has a mouth sore, a white patch, or difficulty opening the jaw that has been present for more than two weeks - do not wait.
Book a consultation with Dr. Supreet Bhatt, Head & Neck Cancer Surgeon in Ahmedabad →
An examination takes under 30 minutes. The information it gives you is permanent.
Dr. Supreet Bhatt is a Head & Neck Surgical Oncologist based in Ahmedabad, Gujarat, with subspecialty training in oral cancers, thyroid cancers, and reconstructive surgery for head and neck cancer patients. For appointments and consultations,
visit drsupreetbhatt.com/oral-cancers-surgeon-in-ahmedabad.

Head and Neck Cancer Surgeon, Senior Consulatent Zydus Cancer Center, Skull base cancer specialist

